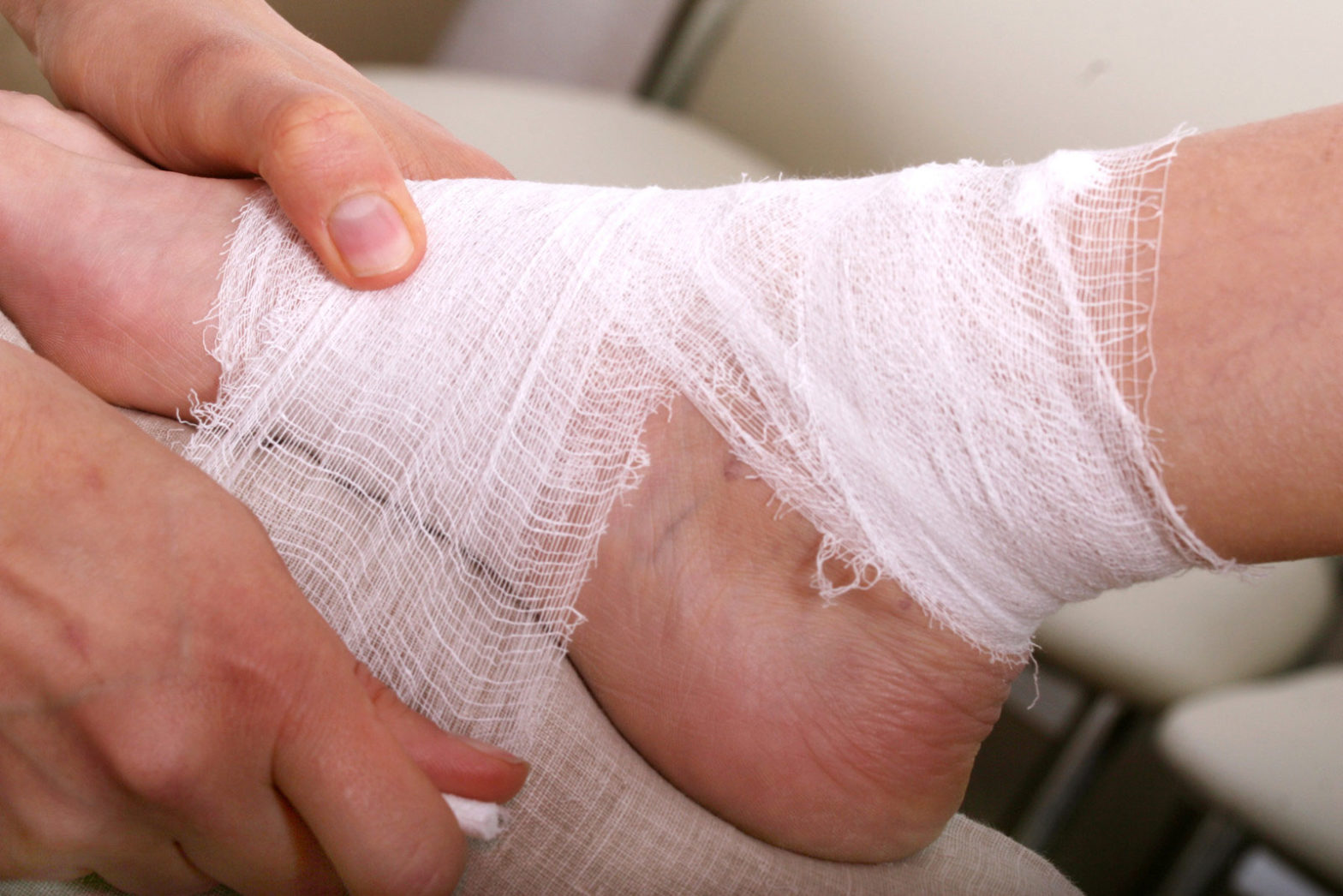
A diabetic foot ulcer is an open sore or wound that occurs in a person with high blood sugar. It is commonly located on the bottom of the foot. All people with diabetes can develop foot ulcers and foot pain, but in some people, the skin does not heal and can progress into an ulcer or infection. According to Michigan Medicine, six percent of those who develop a diabetic foot ulcer will be hospitalized due to infection or other ulcer-related complications. Podiatrists usually work with a team of medical professionals comprising a diabetes specialist, a wound specialist, an infectious disease specialist and a vascular specialist to treat chronic diabetic foot ulcers. As they deal with the challenges of treating non-healing diabetic foot ulcers, podiatric practices can rely on a professional podiatry billing company to streamline their claims processing tasks.
Patients with diabetes are at a higher risk of chronic foot ulcers if they have high blood sugar, nerve damage, foot deformities, or poor circulation. Healing time for foot ulcers depends on a variety of factors, such as wound size and location, pressure on the wound from walking or standing, swelling, circulation, blood glucose levels, wound care, and what is being applied to the wound.
Treatment of a Chronic Diabetic Foot Ulcer
The gold standard for diabetic foot ulcer treatment includes debridement of the wound, off-loading of the ulcer, applying medication or dressings, and preventing infection by keeping the ulcer clean and bandaged.
- Debridement of the wound: A podiatrist will start the treatment with debridement – cleaning the wound and cutting away dead or infected tissue. Debridement is important because dead skin hampers the development of healthy new tissue, and also makes the affected area more vulnerable to infection. Removal of the dead skin will promote healing. Debridement will be done surgically, enzymatically, biologically, or through autolysis.
- Dressings: The wound area is cleaned and a suitable dressing and ointment are put on it. There are different types of diabetic ulcers such as venous ulcers and ischemic ulcers. Podiatrists will apply the most appropriate dressing for the ulcer type. Optimal dressings are those that are free from contaminants, will absorb exudates and toxic elements, maintain a moist environment at the wound interface, and protect surrounding healthy skin. While antimicrobial dressings are used for infected diabetic foot ulcers and ulcers at-risk of infection, daily saline or similar dressings will be used to provide a moist wound environment. High-quality wound care kits can ensure better outcomes.
- Ulcer pressure offloading: Another important part of the treatment is offloading, or taking weight and pressure off the wound. Inadequate off-loading is a significant reason for the delay of ulcer healing. To reduce the pressure and irritation to the ulcer area and speed up the healing process, patients may be asked to wear special footgear, or a brace, specialized castings, or use a wheelchair or crutches. Non-removable total-contact casts (TCCs) are an ideal option for effective off-loading of ulcers located at the forefoot or midfoot. Half shoes, therapeutic shoes, custom insoles, and the use of felted foam are other alternative methods to off-load wounds located on the forefoot.
Other add-on therapies to treat chronicdiabetic ulcers include hyperbaric oxygen therapy and negative-pressure wound therapy (NPWT). Antibiotics will be prescribed if the wound is infected. X-rays of the feet will be taken to check whether any underlying bone is infected or even fractured. If there is any sign of poor blood circulation, surgery will be recommended to open up blood vessels.
During the course of the treatment, the patient’s foot will be regularly evaluated for any redness, inflammation or swelling, as well as any discharge or smell. Patients will be advised to avoid any unnecessary standing or walking with the affected foot, as ulcer cannot heal if it is constantly under pressure. Preventing diabetic foot ulcers reduces associated high morbidity and mortality rates, and the danger of amputation. Having feet screened and assessed every year by a podiatrist will help diabetic patients to prevent ulcers and infections. A foot and ankle surgeon will also take care to manage the patient’s blood glucose and other health problems. Controlling blood glucose level is crucial during the treatment of a diabetic foot ulcer to enhance healing and reduce risk of further complications.
Concierge Wound Care Solutions are available to streamline the wound-care prescription process. This innovative electronic program allows podiatrists to manage their prescriptions online and also ensures timely delivery of wound care supplies to patients.